By Katie Brooks, LCSW
Cognitive Behavioral Therapy (CBT Therapy) is a rapidly growing evidence-based psychotherapeutic treatment that can be used to treat a wide range of mental health issues. Over 400 published empirical studies have consistently demonstrated that CBT is effective for treating depression, general anxiety disorder, panic disorder, social phobia, posttraumatic stress disorder, childhood depressive and anxiety disorders, marital distress, anger, childhood somatic disorders, chronic pain, obsessive-compulsive disorders, bulimia nervosa, and schizophrenia. CBT is collaborative process with practical tools and strategies for solving everyday problems.
CBT is an umbrella term combining many traditional and innovative cognitive and behavioral theories and therapies. It has a rich collection of proven techniques designed to help people challenge negative thoughts, learn positive behaviors, prevent relapse, set goals, regulate emotions, dispute irrational beliefs, and solve problems. CBT interventions help people navigate tough challenges and build happier, more meaningful lives. Newer approaches help people to learn mindfulness skills to become more aware of the present moment and more accepting of unpleasant situations, thoughts, feelings, and behaviors.
Cognitive Therapy
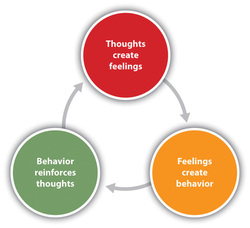
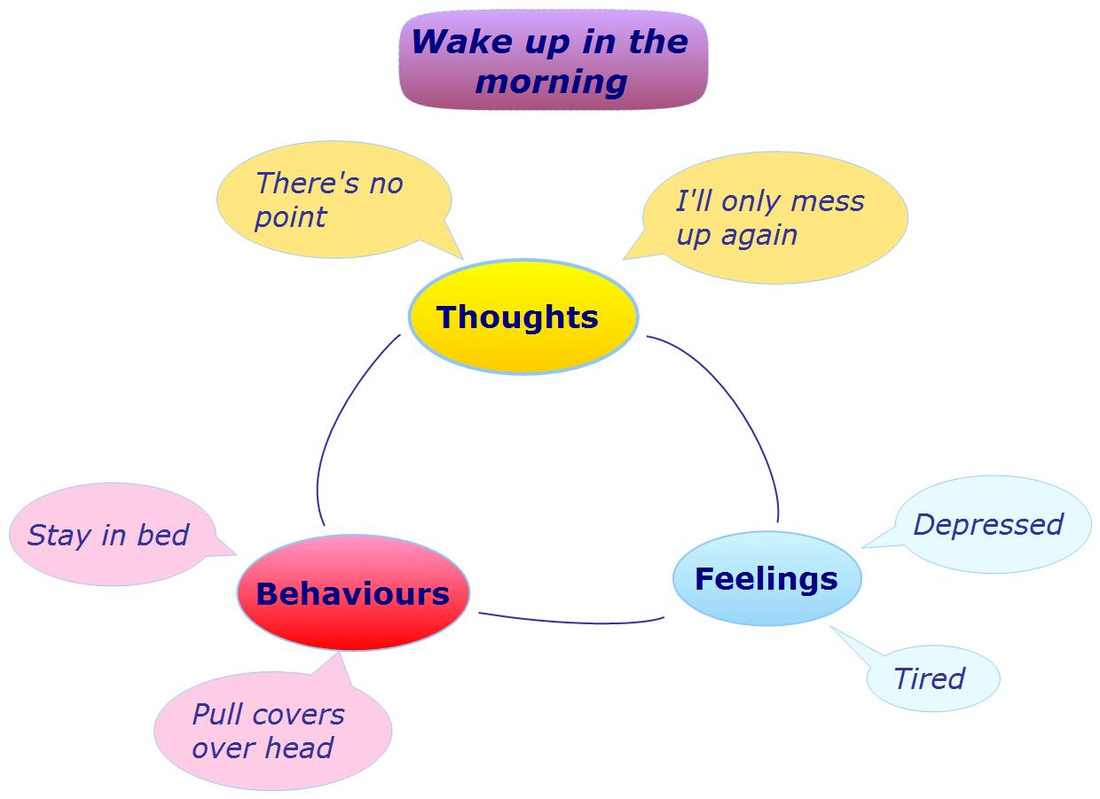
Central to CBT is the role thoughts, feeling, and behaviors play in the development and maintenance of family health, relationship, and mental health problems. Perceptions of daily events and past memories can strongly influence feelings and behaviors. Helping people become more aware of how everyday situations can trigger automatic thoughts, strong emotional feelings and behaviors is key in cognitive therapy. By examining the accuracy of thoughts and beliefs, mental health professionals can help clients develop more realistic and balanced ways of thinking, feeling, and acting.
For example: People stuck in traffic may think: (1) this situation is awful, (2) it’s not fair, (3) why me, (4) other drivers are idiots, and / or (5) bad things only happen to me. These automatic thoughts can make people feel anxious, irritated, frustrated, or annoyed. These negative emotions can trigger relief-seeking behaviors like screaming, pointing, yelling, tailgating, or gesturing. Helping people become aware of the relationship between everyday situations, thoughts, feelings, behaviors, and the body is one of the most important skills to learn in CBT.
According to Dr. Aaron T. Beck, founder of Cognitive Therapy, depressed clients learn and develop automatic negative thoughts and core beliefs about self, others, and the world. Clinicians can help clients discover that these thoughts are not facts even though they may feel and act like they are true. Deeper maladaptive beliefs learned from childhood are at the root of many underlying repetitive presenting and behavioral problems. Setting goals, forming a good therapeutic alliance, and helping people modify their core beliefs are some of the most effective strategies in treatment.
Behavioral Therapies
In addition to Cognitive Therapy Techniques, CBT has a rich tradition of behavioral therapies where the principles of learning are used to help people change self-defeating behaviors. Setting goals and measuring progress are key strategies in behavioral therapies. Top behavioral therapy intervention techniques include: modeling, relaxation training, breathing techniques, systematic desensitization, exposure therapies, assertiveness training, graded task assignment, increasing pleasurable activities, self-esteem training, problem-solving, moderation management skills, self-monitoring techniques, activity scheduling, contingency management techniques, relapse preventing, and coping skills training.
Positive action plans with goals and action steps are key to helping people initiate and maintain lasting behavioral change. To learn new behavioral habits or new skills takes repeated practice, role-play and rehearsal. Practicing small steps over and over again increases self-efficacy and the new habit becomes wired in the brain. We can train our brain to thing, feel, and act differently with repeated practice.
Feeling Better Strategies
CBT can also help people to learn how to regulate emotions and manage their feelings. Clients are sometimes overwhelmed by the unexpected tidal waves of emotional pain. Intense emotional reactions often motivate people to engage in self-defeating, relief-seeking behaviors like avoidance, over-eating, or suicidal behaviors. CBT helps people become more aware of their feelings and how to identify situations that trigger these feelings. Emotional regulation skills, or feeling better strategies, help clients cope with the challenges of everyday life.
CBT and Brain-Based Strategies
Contemporary CBT combines and integrates evidence-based practices from a wide range of approaches including the mind-body connection. Brain based research is charting new territory for mental health professional to use brain-friendly strategies in everyday clinical practice. CBT can help to wire and fire new neurological activity in the brain and help people change the meaning of traumatic memories. With hard work and repeated practice new thoughts, feelings and behaviors can become wired in the brain. Research confirms that the brain continues to heal, grow and develop throughout the life span. Helping people learn more about the brain can help them to learn more effective ways to change thoughts, feelings, and behaviors.
CBT and the Environment
The environment and relationships also have a significant impact on peoples’ thoughts, feelings and behaviors. Improving interpersonal skills can radically improve mood by teaching clients how to cope with dysfunctional family communication patterns and interactions. Family-based interventions help to address some of the potential root causes that exacerbate and maintain a client’s self-destructive patterns. Mental health professionals are challenged to help people learn how to cope with the impact that the environment has on their problems. Relapse is often triggered by high-risk situations and environments that perpetuate self-defeating behaviors. While unaddressed environmental and relationship influences pose significant challenges for both clients and clinicians, advances in CBT integrate strategies that help clients learn to navigate both environmental, family and other relationship challenges. The therapeutic relationship is the ideal place to help people have more effective interpersonal skills.
CBT and the Body
Finally, CBT is increasingly recognizing the way events, experiences, thoughts, feelings and behaviors trigger physical reactions in the body. Significant events like trauma, depression, anger and anxiety produce physical reactions in the body. Some people are better at sensing with their body and benefit more from body-based therapies. Paying attention to body language, facial expressions, and tone of voice are important for mental health professionals. Suggesting physical exercise and increased activity can have amazing psychological and physical results for the client.
CBT in a Nutshell
In short, CBT can help people develop new coping skills, improve relationships, overcome fears, improve mindfulness skills, develop greater acceptance, challenge irrational beliefs, and build happier more meaningful lives. CBT is a collaborative therapy designed to help clients explore options, set goals, and solve problems. While not a magic bullet, CBT provides hope everyday to people facing some of life’s toughest challenges.
Cognitive Behavioral Therapy (CBT Therapy) is a rapidly growing evidence-based psychotherapeutic treatment that can be used to treat a wide range of mental health issues. Over 400 published empirical studies have consistently demonstrated that CBT is effective for treating depression, general anxiety disorder, panic disorder, social phobia, posttraumatic stress disorder, childhood depressive and anxiety disorders, marital distress, anger, childhood somatic disorders, chronic pain, obsessive-compulsive disorders, bulimia nervosa, and schizophrenia. CBT is collaborative process with practical tools and strategies for solving everyday problems.
CBT is an umbrella term combining many traditional and innovative cognitive and behavioral theories and therapies. It has a rich collection of proven techniques designed to help people challenge negative thoughts, learn positive behaviors, prevent relapse, set goals, regulate emotions, dispute irrational beliefs, and solve problems. CBT interventions help people navigate tough challenges and build happier, more meaningful lives. Newer approaches help people to learn mindfulness skills to become more aware of the present moment and more accepting of unpleasant situations, thoughts, feelings, and behaviors.
Cognitive Therapy
Central to CBT is the role thoughts, feeling, and behaviors play in the development and maintenance of family health, relationship, and mental health problems. Perceptions of daily events and past memories can strongly influence feelings and behaviors. Helping people become more aware of how everyday situations can trigger automatic thoughts, strong emotional feelings and behaviors is key in cognitive therapy. By examining the accuracy of thoughts and beliefs, mental health professionals can help clients develop more realistic and balanced ways of thinking, feeling, and acting.
For example: People stuck in traffic may think: (1) this situation is awful, (2) it’s not fair, (3) why me, (4) other drivers are idiots, and / or (5) bad things only happen to me. These automatic thoughts can make people feel anxious, irritated, frustrated, or annoyed. These negative emotions can trigger relief-seeking behaviors like screaming, pointing, yelling, tailgating, or gesturing. Helping people become aware of the relationship between everyday situations, thoughts, feelings, behaviors, and the body is one of the most important skills to learn in CBT.
According to Dr. Aaron T. Beck, founder of Cognitive Therapy, depressed clients learn and develop automatic negative thoughts and core beliefs about self, others, and the world. Clinicians can help clients discover that these thoughts are not facts even though they may feel and act like they are true. Deeper maladaptive beliefs learned from childhood are at the root of many underlying repetitive presenting and behavioral problems. Setting goals, forming a good therapeutic alliance, and helping people modify their core beliefs are some of the most effective strategies in treatment.
Behavioral Therapies
In addition to Cognitive Therapy Techniques, CBT has a rich tradition of behavioral therapies where the principles of learning are used to help people change self-defeating behaviors. Setting goals and measuring progress are key strategies in behavioral therapies. Top behavioral therapy intervention techniques include: modeling, relaxation training, breathing techniques, systematic desensitization, exposure therapies, assertiveness training, graded task assignment, increasing pleasurable activities, self-esteem training, problem-solving, moderation management skills, self-monitoring techniques, activity scheduling, contingency management techniques, relapse preventing, and coping skills training.
Positive action plans with goals and action steps are key to helping people initiate and maintain lasting behavioral change. To learn new behavioral habits or new skills takes repeated practice, role-play and rehearsal. Practicing small steps over and over again increases self-efficacy and the new habit becomes wired in the brain. We can train our brain to thing, feel, and act differently with repeated practice.
Feeling Better Strategies
CBT can also help people to learn how to regulate emotions and manage their feelings. Clients are sometimes overwhelmed by the unexpected tidal waves of emotional pain. Intense emotional reactions often motivate people to engage in self-defeating, relief-seeking behaviors like avoidance, over-eating, or suicidal behaviors. CBT helps people become more aware of their feelings and how to identify situations that trigger these feelings. Emotional regulation skills, or feeling better strategies, help clients cope with the challenges of everyday life.
CBT and Brain-Based Strategies
Contemporary CBT combines and integrates evidence-based practices from a wide range of approaches including the mind-body connection. Brain based research is charting new territory for mental health professional to use brain-friendly strategies in everyday clinical practice. CBT can help to wire and fire new neurological activity in the brain and help people change the meaning of traumatic memories. With hard work and repeated practice new thoughts, feelings and behaviors can become wired in the brain. Research confirms that the brain continues to heal, grow and develop throughout the life span. Helping people learn more about the brain can help them to learn more effective ways to change thoughts, feelings, and behaviors.
CBT and the Environment
The environment and relationships also have a significant impact on peoples’ thoughts, feelings and behaviors. Improving interpersonal skills can radically improve mood by teaching clients how to cope with dysfunctional family communication patterns and interactions. Family-based interventions help to address some of the potential root causes that exacerbate and maintain a client’s self-destructive patterns. Mental health professionals are challenged to help people learn how to cope with the impact that the environment has on their problems. Relapse is often triggered by high-risk situations and environments that perpetuate self-defeating behaviors. While unaddressed environmental and relationship influences pose significant challenges for both clients and clinicians, advances in CBT integrate strategies that help clients learn to navigate both environmental, family and other relationship challenges. The therapeutic relationship is the ideal place to help people have more effective interpersonal skills.
CBT and the Body
Finally, CBT is increasingly recognizing the way events, experiences, thoughts, feelings and behaviors trigger physical reactions in the body. Significant events like trauma, depression, anger and anxiety produce physical reactions in the body. Some people are better at sensing with their body and benefit more from body-based therapies. Paying attention to body language, facial expressions, and tone of voice are important for mental health professionals. Suggesting physical exercise and increased activity can have amazing psychological and physical results for the client.
CBT in a Nutshell
In short, CBT can help people develop new coping skills, improve relationships, overcome fears, improve mindfulness skills, develop greater acceptance, challenge irrational beliefs, and build happier more meaningful lives. CBT is a collaborative therapy designed to help clients explore options, set goals, and solve problems. While not a magic bullet, CBT provides hope everyday to people facing some of life’s toughest challenges.

 RSS Feed
RSS Feed
